Dopamine Hydrochloride: Substance With a Past, Present, and a Future in Medicine
Historical Development
Dopamine hydrochloride started its journey in the mid-twentieth century, stepping straight into the heart of modern medicine. The fascination with dopamine itself goes further back, when brain chemistry was mostly a guessing game. Early researchers poking around with animal brains started identifying compounds like dopamine and norepinephrine, trying to pin down their roles. By the time dopamine hydrochloride made its way into hospital crash carts, the world was already focused on so-called “chemical messengers” in the human body and their influence on behavior, mood, and disease. This push to understand neurotransmitters led to the rapid isolation and synthesis of dopamine for clinical use. Experienced paramedics and ICU doctors will tell you—dopamine shows up in some of the most critical moments of their careers, especially when a patient's blood pressure refuses to budge. The therapeutic value wasn’t just plucked out of thin air; it stemmed from a mix of desperate clinical need and persistent lab chemistry, followed by rigorous studies in the 1960s and '70s. Dopamine hydrochloride found its place in emergency and intensive care, a direct result of this history of scientific trial and real-world necessity.
Product Overview
People in medicine often think of dopamine as a neurotransmitter, but the hydrochloride salt serves a different set of purposes outside the brain. This isn’t about mood or pleasure circuits; it’s about keeping vital organs perfused. The injectable product arrives as a sterile solution tailored for intravenous use, stabilizing people in shock, whose bodies teeter between life and death. For nurses and critical care physicians, dopamine hydrochloride is a means to jolt flagging hearts and maintain blood flow to the kidneys and brain. Unlike more common oral medications, it doesn’t land on drugstore shelves, nor is it something folks sit around discussing unless they work very close to the edge of medicine. Available in various concentrations, this pharmaceutical-grade compound gets added to IV lines under close monitoring. The convenience and impact of this drug stem from both its predictable response in the human body and its long history of tracked outcomes.
Physical & Chemical Properties
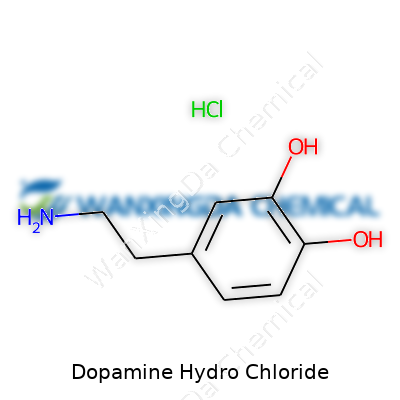
The compound sits in vials and ampoules as a crystalline white powder or appears as a clear, colorless solution. Many pharmacists have commented on the ease with which dopamine hydrochloride dissolves in sterile water or saline—a testament to its chemical stability under standard conditions. It carries the chemical formula C8H12ClNO2, jobbed with a hydrochloride group that makes it more soluble for injection, a simple twist to a naturally occurring molecule with life-saving impact. There's no smell, nothing showy about its appearance, but once inside an IV bag, this simple molecule gets busy. Its half-life in the bloodstream hovers below a few minutes, driving the need for continuous infusion instead of intermittent dosing. That short window has shaped not only how clinicians administer the drug but also how closely patients are watched after it goes in.
Technical Specifications & Labeling
Anyone familiar with hospital pharmacies recognizes the telltale labels—clear dosing ranges, explicit reminders about dilution, protection from light, and warnings about extravasation risks. It’s hard to overstate the importance of accuracy in labeling, given the drug's narrow therapeutic window and the need for individualized titration. Even seasoned nurses double-check dopamine orders, knowing it can interact with other common ICU drugs and rapidly change blood pressure. Packaging usually favors single-dose vials, with printed concentrations that cut down on dosing mistakes. With so much riding on a clear label, regulatory agencies worldwide keep a tight grip on naming conventions and instructions to avoid confusion in an already tense environment.
Preparation Method
Manufacturing dopamine hydrochloride isn’t a matter of mixing and shaking. Precise synthesis typically starts from L-tyrosine, an amino acid found in food and already involved in human metabolism. Chemical engineers leverage multi-step methods—enzymatic hydroxylation transforming L-tyrosine into L-DOPA, then decarboxylation leading to dopamine. Adding the hydrochloride involves a controlled acid-base reaction, followed by crystallization, drying, and repeated purification. Quality control labs run samples through rigorous assays, confirming purity and concentration to the parts-per-million. In hospitals, the last stage is more mundane: dissolving the powder into exactly the right volume of saline or dextrose and labeling it for rapid delivery to a patient in crisis.
Chemical Reactions & Modifications
Once synthesized, dopamine hydrochloride isn’t especially reactive under normal storage conditions, making it a safe and predictable pharmaceutical. Researchers have played with chemical modifications, sometimes tweaking the amine or catechol groups to see if they can unlock better receptor selectivity, longer duration, or reduced side effects. These chemical explorations have led to analogues but none that fully replace the straightforward action of classic dopamine. The pharmaceutical industry has learned to respect the original, keeping changes minimal outside of formulation improvements aimed at reducing contamination or improving solubility. Labs keep exploring, always hoping for a new twist that might make this old standby just a little gentler on fragile patients.
Synonyms & Product Names
Names like “Dopamine hydrochloride,” “Intropin,” and occasionally “Dopamine HCl” circle around this compound in drug dictionaries, hospital formularies, and emergency training manuals. Academic literature and clinical guidelines often default to the simplest moniker, avoiding confusion during stressful events. Some countries approve other branding, but naming standards usually focus on clarity over marketing flash. For folks working in clinical settings, what matters is the unmistakable message delivered by standardized labels and straightforward instruction sheets, the kind that cut through the fog when seconds count.
Safety & Operational Standards
Safety systems around dopamine hydrochloride didn’t arise by accident. Toxic effects at the site of injection, like tissue necrosis after a rogue IV, have prompted strict administration protocols. Dilution errors or accidental boluses can swing blood pressure from dangerously low to sky-high without warning. Standardized training for ICU and ER staff includes careful pump programming and double-verification systems. Manufacturers conduct extra sterility and stability testing, aware that even a minor deviation in pH or contamination level could jeopardize a desperately ill patient. Regulatory oversight ensures that only reputable suppliers sell the drug, with batch testing and post-market surveillance acting as backstops. These layered safeguards are the reason dopamine remains widely trusted even as more targeted drugs have entered the scene.
Application Area
Dopamine hydrochloride fills a niche in modern hospitals, especially for patients whose bodies stop responding to less intense medicines. It’s given when heart failure or shock shrinks blood flow to major organs. Critical care, cardiology, nephrology—all claim a piece of its history, but nowadays its use is tightly rationed. Guidelines stress the risk of arrhythmia, tachycardia, and peripheral vasoconstriction. Team huddles in the ICU swirl around these side effects, balancing the urge to restore blood pressure against the real chance of complications. In clinical practice, dopamine sometimes recedes into the background behind newer agents like norepinephrine, but it remains a core part of training for everyone who sets foot in an intensive care ward.
Research & Development
Innovation keeps circling around dopamine and its relatives, driven by the unending chase for safer, smarter drugs. Biomedical research hammers away at the same questions year after year: can a chemical tweak minimize arrhythmias, extend the half-life, or make administration smoother? Decades of clinical trials fill the medical literature, some painting dopamine hydrochloride as indispensable, others nudging practitioners toward alternatives as evidence on outcomes shifts. Scientists studying dopamine’s metabolic role beyond the acute care word still hope for insights that might transform chronic disease treatment too. Research into better formulations and delivery systems continues in the hope of reducing dosing errors and minimizing complications in the heat of a code.
Toxicity Research
Long before any modern approval came, animal studies and human trials flagged dopamine’s powerful punch. The toxicity profile shows a sharp line: below a certain dose, it supports organs, above it—arrhythmias, chest pain, runaway blood pressure, and local tissue death from accidental extravasation. Standard treatment guidelines reflect the lessons hammered out in practice and in lab studies. Medical journals have documented catastrophic complications, leading to increased awareness and practical interventions like carefully titrated infusion pumps, robust monitoring protocols, and fallback strategies for unexpected drug reactions. Staff training now parallels the evolution of research, using real-case scenarios to make sure everyone can spot and respond to danger quickly.
Future Prospects
Chemical history shows that no drug, no matter how storied, holds its crown forever. Dopamine hydrochloride now faces competition from newer molecules designed for sharper selectivity or fewer adverse effects. Large trials and evolving treatment protocols push clinicians to reassess traditional drugs, often moving toward agents that provide a gentler hemodynamic lift. At the same time, emerging research keeps dopamine relevant for special cases, particularly in under-resourced settings where alternatives may not be as available. The future likely holds a role for dopamine as both a backup and as a research tool revealing new angles on its role in the human body. Payers, regulators, and health systems will have to weigh these evolving roles as evidence shifts and new molecules reach the bedside. For now, as more innovations filter through hospitals and research pipelines, dopamine hydrochloride continues to anchor protocols that have saved countless lives across decades.
Straight Talk About Its Uses
Dopamine Hydrochloride stands out in medicine because it does something that modern-day drugs don’t always pull off—fast, targeted action for folks in crisis. Hospitals keep this drug handy for one main reason: it keeps the blood flowing when someone’s life depends on it. Heart failure, low blood pressure after surgery, shock—a nurse once told me these are moments you see the value of what seems like an old-school drug.
Real-World Stakes in Critical Care
Let’s drop the jargon. If someone’s heart is failing or their blood pressure drops dangerously, the body can’t deliver oxygen to organs. I spent hours on heart units, and more than a few times watched doctors order Dopamine Hydrochloride as a last push to keep kidneys and brain from shutting down. The drug tells blood vessels to squeeze just enough so pressure stays up, and it nudges the heart to beat stronger.
In emergencies, there’s almost no room for error. Doctors and nurses rely on medication they trust. And Dopamine Hydrochloride earns that trust the old-fashioned way: it works fast, and you can see the difference on heart monitors and patient faces. This is not yesterday’s medicine—it still plays a serious part in saving lives.
Understanding How It Works
You don’t need a PhD to get the point. Dopamine is a natural chemical your body uses to signal nerves. When the hospital gives it as Dopamine Hydrochloride, they use a pump that can match your needs minute by minute. Low dose, blood flow gets a gentle push. Higher amounts, the heart puts in more work. The real skill comes in knowing how much to give, since too little might change nothing—and too much can cause fast, erratic heartbeats or even restrict blood to the hands and feet.
Why Hospitals Still Use It
It’s important to question why a drug sticks around when fancier options hit the market all the time. Dopamine Hydrochloride often steps in for people in septic shock when other medicines don’t seem to cut it. In smaller hospitals, where every dollar spent counts, Dopamine brings reliability that’s tough to replace. A 2021 review in the journal “Critical Care” still lists it among recommended picks in certain tricky cases.
Doctors also know how to use it. That matters a lot more than people realize, especially in places with less staff training. There are risks—abnormal rhythms, headaches, problems with the IV line—but teams learn to spot them. Emergency care always means choices, and Dopamine gives another option.
Questions for the Future
Some medical pros talk about moving away from Dopamine in favor of new drugs like norepinephrine, which can have fewer side effects. Still, research doesn’t call for banning Dopamine altogether. The question is really about using it at the right time, for the right patient. That’s where teaching and training matter.
Better outcomes also come from testing new drugs head-to-head, including with folks who have kidney or heart problems. As more hospitals review their drug use and update guidelines, there’s a strong case for keeping Dopamine Hydrochloride available, and making sure staff can handle it safely. No matter how medicine changes, some tools just work—that’s the lesson this drug keeps teaching.
Understanding the Realities Behind Dopamine Treatment
Dopamine Hydrochloride often steps in for people in trouble—serious kinds of trouble—like shock where blood pressure crashes and organs cry out for oxygen. This isn’t a medicine you take to feel better after a cold. This is hospital stuff, delivered through tubes, usually when seconds count and lives hang in the balance. Yet, even when a drug saves lives, it can take its own toll. That makes it important to talk honestly about those side effects, especially since so many folks in crisis aren’t in any shape to ask questions.
What Happens to the Body?
Dopamine Hydrochloride works by tightening the blood vessels and pushing up the heart’s pumping strength. When I worked alongside nurses and physicians on cardiac units, we always kept a sharp eye on anyone hooked up to this medicine, because things can swing quickly. One common problem is a pounding heartbeat. People sometimes feel their chest thumping, or the monitor jumps with tall spikes. That’s because dopamine doesn’t just wake up sluggish blood flow—it can overstimulate the body as well.
Besides racing heartbeats, blood pressure can shoot up, especially if the dose isn’t right. For some folks, that creates headaches that just won’t quit, or in rare situations, chest pain. I’ve seen cases where pressure kept climbing and landed the patient in more trouble than before. Blood vessels everywhere tighten, and in fragile people, that leaves toes or fingers turning cold or blue. That’s a warning sign: circulation isn’t reaching every corner.
Beyond the Heart: Other Signs to Watch
Restlessness and anxiety show up in many patients I’ve looked after. You lie there, worried and confused, sometimes shaky, sometimes even nauseous. Vomiting tends to creep in, and you can’t always guess when or why. If kidneys or other organs already have trouble, dopamine changes in blood flow might make things worse, though sometimes it helps. The body works like a chain—a tug in one spot rattles the entire system.
Knowing the Risks, Asking Better Questions
One thing that sticks with me: Every patient brings their own strengths and weaknesses to the hospital. A person with hardened arteries faces higher risks with this drug. If you already have rhythm trouble in your heart, dopamine can stir up dangerous arrhythmias. On top of that, anyone with a swollen or infected vein from a poorly placed IV may suffer tissue damage if dopamine slips out of the vein. That turns into a medical emergency fast.
Patients and families don’t always get briefed on all these possible shocks—life is moving too quickly, rooms are crowded, alarms are ringing. But knowing these side effects matters. It allows people to point to something that doesn’t feel right, and health workers can catch dangerous trends earlier.
Better Monitoring, Clearer Communication
To soften the risks, strict monitoring means everything. Nurses and doctors check blood pressure, heart rate, oxygen numbers, and keep an eye for cool or dusky fingers and toes. Hospital teams also rotate IV sites and flush lines carefully. If problems crop up, the team switches gears fast, tweaking drugs or using different therapies. In my experience, the more everyone shares information—from nurses at the bedside to family members noticing mood changes—the better patients do, even with a medicine this powerful.
Real-World Decisions In the Emergency Room
Eyes dart from monitors to the patient. Every decision counts. Dopamine hydrochloride isn’t just another drug collecting dust on the shelf—it’s rescue in a vial when a patient’s blood pressure plummets. I’ve watched the look on nurses’ faces when a doctor calls for dopamine. Everybody knows someone just got a second shot at staying alive.
Administration Isn’t Casual
Most folks never see or hear about dopamine hydrochloride unless they’re in a critical care unit. Doctors don’t hand this out for headaches or run-of-the-mill fatigue. Instead, it’s deployed for stubbornly low blood pressure, for cardiac arrest, for the moments where a failing heart threatens to shut the system down. In these moments, dopamine becomes a lifeline.
Medicine gets delivered in ways that match the urgency. For dopamine, the most reliable path is straight into a vein. Nurses set up an intravenous (IV) infusion—not a quick injection. The drug enters the bloodstream drop by drop from a bag, through plastic tubing and a needle or catheter. Watchful eyes check monitors as doses get fine-tuned. The aim is to boost blood flow and bring back the pressure, but not so much that the heart races dangerously or starts skipping beats.
The Human Touch Behind the Machine
It’s easy to see the machines and miss the skill involved. A nurse adjusts the IV rate, checking for reactions. A doctor keeps an eye on urine output and heart rhythm. Too little dopamine, no effect; too much, the cure becomes a new danger. I once saw a team pull together, debating the next steps while the patient’s family paced outside. They calibrated every milliliter as if the next tweak might change the outcome—because it might.
Why Strict Monitoring Matters
All the focus on dosage isn’t just cautiousness. Dopamine can push blood pressure up and help the kidneys keep filtering waste. Give too much, though, and you might see arrhythmias—the kind that shake confidence fast. Nurses and doctors hook up patients to machines, double-checking everything from blood pressure to the way urine looks. In that blend of vigilance and experience, the value of the team shows up. Data from decades of use supports this approach—there’s no easy substitute.
Facing Shortages and Training Gaps
Every so often, hospitals run short on these critical drugs. Then the scramble begins—what’s the alternative? Norepinephrine gets used in some of the same situations, but it isn’t exactly a twin. Training new staff matters more than any protocol; mistakes with dopamine can be costly in seconds. I’ve seen senior nurses quietly coaching rookies, walking them through the mixing and pump programming at two in the morning. The right habits and knowledge matter just as much as having dopamine on the shelf.
Better Tools and Next Steps
Continuous education stands as the best fix. It’s not the machines or even the latest research, useful as those are, but people staying sharp. Hospitals do their best to keep simulations and refresher courses ongoing, teaching staff how to recognize side effects fast and adjust dosing without delay. For this drug, experience isn’t just useful—it’s a necessity in turning potential into results, especially when stakes soar.
Dopamine hydrochloride, in the end, isn’t handled lightly. It calls for know-how, judgment, and teamwork—the kind of things that don’t show up on a pharmacy label, but save lives all the same.
A Look at the Drug’s Strong Effects
Nobody forgets the first time they see dopamine hydrochloride used in a critical care unit. The atmosphere tenses up as the nurse spikes the bag and prepares the line. Dopamine isn’t a routine remedy. It can spark life back into a failing heart, but not without risks. Fast drops in blood pressure, pounding heartbeats, and racing signals through the nervous system don’t leave much margin for error. These are not just footnotes in the drug reference book; they are moments staff feel at the bedside.
Why Precision Is Non-Negotiable
In my experience working alongside emergency and ICU teams, nobody rolls the dice with dopamine. The dose often must fit the patient’s unique needs—tiny mistakes swing the results wildly. Precision matters for everything: heart rhythms, blood flow to the kidneys, and brain perfusion can each change as the infusion rate shifts. Clinical guidelines urge minimum doses that still keep pressure up. Pushing levels too high sets off rapid heart rhythms or, worse, puts the patient at risk for tissue damage.
People sometimes think, “More medicine, faster results.” Dopamine hydrochloride does not work that way. The wrong amount at the wrong time results in harm. Overloading the veins in fragile people leads to chest pain, arrhythmias, even limb loss from too much vasoconstriction. Experience shows caution always wins out when life is on the line.
Watching for Invisible Dangers
Dopamine isn’t just about numbers. It can interact with other drugs used for critical care, risking dangerous swings in heart rate or blood pressure. Patients who already take monoamine oxidase inhibitors come to mind. Combining the two leads to an overpowering surge—something best avoided in already unstable patients.
Kidney function also changes with dopamine. There’s still debate on whether it truly protects the kidneys in shock. What’s certain: any sign of poor urine output or electrolyte swings needs a fast response, not just a hope that dopamine does the trick. Regular labs, close nursing checks, and communication keep things on the right track.
Seeking Better Paths
Some doctors look at dopamine as old-school therapy. Newer drugs target problems more precisely with fewer risks. But for places without those options, dopamine serves as a lifeline. That points toward a bigger need: better education, updated protocols, and clear guidelines. Every hospital benefits from organized teaching on handling drugs with narrow margins like this one. Peer-reviewed studies should guide dosing, monitoring, and prevention of complications. Institutions can schedule mock code drills that include dopamine use to sharpen judgment under stress.
If there’s one lesson I’ve learned, it’s this: even the strongest medicine can do harm without the right respect and know-how. Dopamine hydro chloride holds power; using it safely demands not just technical skill but a deep sense of vigilance and teamwork.
Looking Beyond the IV Drip
Dopamine hydrochloride tends to show up in emergency rooms as the last hope for people with dangerously low blood pressure or weak heartbeats. It gets pumped into veins with the doctor’s order and close monitoring. Whenever a person’s life is at stake, few care about anything other than the next minute. Yet, this medication’s story doesn’t end at its primary job—there’s a real problem lurking under the surface, and that’s the way it can mix with other drugs already in the patient’s system.
Real-Life Risks in Busy Hospitals
Hospitals are busy places. Patients, especially in critical care, might have a lineup of medicines entering their bloodstream. Doctors and pharmacists keep lists and charts, but no protocol can outrun the speed at which emergencies unfold. Dopamine hydrochloride doesn’t play nicely with everything, and doctors know this from both textbooks and tough nights on call. The risk of drug interactions doesn’t just come from books; I have spent time with medical teams watching them review every line of an admission chart, looking for hidden dangers.
The Messy Side of Mixing Medications
Dopamine hydrochloride can react badly with a variety of medications. Take monoamine oxidase inhibitors for depression—combine these with dopamine hydrochloride, and you can end up with a runaway blood pressure crisis. Blood thinners, anesthetics, some antidepressants, and even cold remedies can cross paths with dopamine, causing trouble or unpredictable reactions. Those little pills often seem harmless, and patients might forget to mention over-the-counter drugs or herbal remedies. It’s easy to see how something slips through the cracks. If a person on blood pressure medicine ends up in the ER and gets dopamine, old notes might not be right up front. The consequences can get serious—dangerously high or low blood pressure, erratic heart rhythms, loss of blood flow to vital organs.
The Weight of Responsibility
Doctors carry the responsibility, but the patient’s role matters, too. Realistically, someone who winds up in shock or cardiac crisis can’t always rattle off every pill they’ve taken that month. Usually, the burden lands on clinicians to ask the right questions, check pharmacy records, and talk with family. Hospital pharmacists remain one of the hidden defenses, often ringing alarms when combinations look risky. I’ve seen a quick phone call to the pharmacy make the difference between a safe recovery and a dangerous spike in blood pressure.
Making Safety Routine, Not Aspirational
Some hospitals use automated systems that flag risky interactions. Others lean on checklists and roundtable discussions among the care team. It sounds like common sense, but even the best teams have to fight time pressure, missing lab data, and incomplete histories. The key solution lies in better communication—reminding patients and families that every prescription and herbal supplement counts, and urging teams to treat medication lists as living documents that evolve with the patient’s hospital journey. Technology can help highlight risks, but people—especially pharmacists—still pick up on nuances the software may miss.
The Real World Isn’t Neat
Dopamine hydrochloride sits at a crossroads between lifesaver and risk. It works wonders against low blood pressure, but the possibility for harm grows with each additional medicine in a person’s system. No amount of software or paperwork fully replaces the vigilance needed from everyone involved. In messy, crowded ERs or ICUs, tiny everyday choices—checking a list twice, making a quick phone call, asking a patient about their last cold pill—protect lives where chemical interactions threaten to end them.