Tyramine: Context, Chemistry, and Consequences
History Turns on the Wheel of Discovery
Tyramine doesn’t often make the daily news, but it carries a resume thick with science and controversy. Discovered by German chemist Baeyer in the late 1800s, its story intertwines with the birth of organic chemistry and the evolution of our understanding of natural amines. Tyramine turns up in fermented foods as a result of protein breakdown, which caught the eye of both food scientists and medical doctors. In the pre-antibiotic era, efforts to explore natural compounds like tyramine shaped pharmacology and biochemistry, setting the stage for discoveries about how small molecules could impact humans far down the line. The path from its isolation to today's deeper studies charts the rise in knowledge about how diet influences the body, especially for those dependent on certain medications.
A Quick Look at Tyramine’s Chemical Makeup
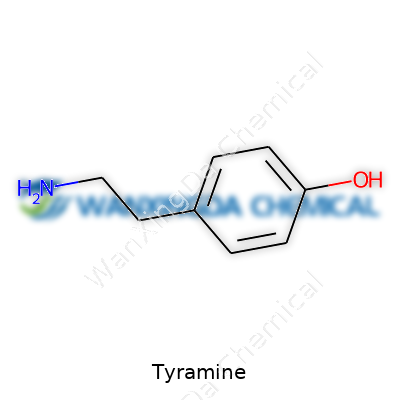
At its core, tyramine comes across as a simple structure: it carries a benzene ring adorned with a hydroxyl group and an amino group, making it a classic aromatic amine. Its chemical formula, C8H11NO, colors its interaction with both water and organic solvents. The substance appears as colorless crystals or a white powder, sharp and bitter on the tongue. Slip it into solution, and it shows moderate solubility in water. Under the microscope, the structure isn’t just for looks — that arrangement tugs at transporters, receptors, and enzymes within our bodies, particularly monoamine oxidase, which holds the key to many of the health concerns surrounding tyramine.
Lab Labels and Practical Details
On labels, tyramine is best known as 4-hydroxyphenylethylamine, showing its close relation to both phenethylamine and other neurotransmitters. Its standardized measures in chemistry circles involve attention to melting point, solubility, and purity, often above 98 percent for research use. Analytical chemists praise its clean melting range from about 163 to 165°C, which speaks to its stable, well-ordered crystal lattice. Labels warn of light and air sensitivity, and proper sealing prevents degradation. Regulations in laboratories keep an eye on exposure since its presence can trigger reactions in some patients and pose contamination problems in sensitive environments.
Crafting Tyramine: From Synthesis to Natural Production
In nature, tyramine forms through the enzymatic decarboxylation of the amino acid tyrosine, mainly by microbes during fermentation. This biochemical side street explains its buildup in cheeses, wines, soy, and even some pickled goods. Industrial chemists can build tyramine in the lab through reduction and decarboxylation paths, often starting from tyrosine or cinnamic acid derivatives. The ease of synthesis compared to some specialty amines gives it a clear presence not only in food science but also in general organic chemistry research. Microbial fermentation piles on more layers: some strains produce more tyramine, and genetically tweaking these organisms brings both solutions and risks for food technologists.
Reactivity and Modifications: The Chemistry Classroom
Reactions involving tyramine generate plenty of conversation among organic chemists. Its amine group serves as a nucleophile in alkylation, and the phenol moiety can undergo electrophilic substitution, much like its cousins in the phenol family. Researchers use these sites for derivatization, tagging tyramine to probes in biological assays or spinning off structural analogs with new pharmacological profiles. Enzymatic processes modify tyramine into various metabolites, showing pathways toward both detoxification and formation of potentially bioactive compounds. Ongoing chemical tinkering helps unearth new uses, especially in analytical and pharmaceutical labs keen on expanding the amine’s range.
Names: Tyramine and Its Chemical Relatives
Beyond “tyramine,” scientists sometimes call it para-tyramine, p-hydroxyphenylethylamine, or 4-hydroxyphenylethylamine. Pharmacology and food chemistry circles flip through these names easily. Given the structure’s similarity to other neurotransmitters, conversations about tyramine can blur into talks on dopamine and phenethylamine, where small tweaks make big differences in biological effects. On ingredient lists in the food trade, though, “tyramine” tends to carry the weight, especially after warnings about its effects for people taking certain medicines.
Safety Standards and Real-World Practice
Tyramine rarely causes trouble for most people. For folks on monoamine oxidase inhibitors (MAOIs), trouble starts with a sharp headache — sometimes much worse. These medicines keep the body from breaking down dietary amines, letting levels spike after a meal rich in tyramine. Doctors call this the “cheese reaction” after old reports of patients suffering from hypertension after nibbling cheese with their pills. Standard operating practices in both pharmacy and food industries warn those at risk, pushing clear labeling and public education. Safe handling in production facilities might draw mostly from standard protocols, given the compound’s low volatility and toxicity for handlers, though strict attention helps avoid cross-contamination and unnecessary occupational exposure.
Field of Use: Medicine Meets Food Science
Tyramine’s main role outside the lab emerges in food and medicine. Fermented foods, especially aged cheeses, cured meats, and certain wines, pack more tyramine due to microbial action. In nutrition and dietetics, this links to patient counseling, particularly for those managing mood disorders or hypertension with MAOIs. Beyond clinical settings, tyramine’s presence in foods kicks off research in food safety, spoilage control, and shelf-life extension. Regulatory bodies weigh research results to set guidelines and enforce safety communications. Some evidence hints at roles in neurotransmitter modulation, though the body’s ability to neutralize small doses usually prevents lasting effects.
What the Scientists Are Chasing: R&D and Toxicity Concerns
Research into tyramine’s effects continues, largely spurred by rising use of antidepressants in aging populations. Scientists check blood pressure effects, track headaches and investigate possible links to migrainous syndromes. Advances in analytical chemistry pinpoint tyramine concentrations down to milligrams per kilogram in foods, helping identify previously overlooked sources. Microbiologists look at fermentation to change tyramine profiles in foods, even aiming for breed-specific cheese cultures to cut consumer risk. Clinical researchers track long-term results in people with limited ability to degrade tyramine, teasing apart genetic and drug-induced aspects of individual sensitivity.
On the toxicology front, acute tyramine poisoning remains rare but frightening. At high doses, vasoconstriction, increased heart rate and dangerous spikes in blood pressure fill out the risk picture. Controls in the medical and food supply sectors focus on education and clear warning systems, since a handful of foods can deliver far more tyramine than others. Newer research checks interactions with other drugs and searches for non-hypertensive adverse effects. Yet it’s worth noting: the vast majority of the population, eating a variety of foods, rarely sees a problem unless sensitive or medicated.
The Road Ahead: Future Outlook
With ongoing interest in functional foods and personalized nutrition, tyramine finds a place in wider conversations about the relationship between what we eat and how it interacts with our bodies. Food science looks towards improved fermentation control and routine screening for amine levels, pressing for technologies that monitor and standardize tyramine content in commercial products. In the realm of mental health, better patient education around tyramine-restricted diets now competes with pharmaceutical companies looking to bring MAOI alternatives, making the need for public awareness all the more important. Genetic testing for individual tyramine sensitivity could arrive soon; in the meantime, sharp attention to labeling and best practices in both food prep and pharmacy help protect those at risk. As science unpacks more about this amine, both opportunities and new responsibilities will pile up, binding together the journey from microbe to meal to hospital ward.
Seeing Tyramine on the Label
Tyramine has a name that usually triggers confusion outside of science circles. Few folks can point it out on a nutrition label, yet this little molecule crops up in foods many people eat each day. Cheddar cheese, cured meats, soy products, even overripe bananas—these all show up with notable amounts. So, what gives tyramine its significance, especially in medicine and health?
Where Tyramine Comes Into Play
Tyramine springs from the natural breakdown of the amino acid tyrosine, which lives in many protein-rich foods. As foods age or ferment, levels climb. People learned centuries ago that some dishes—blue cheese, salami, pickled herring—pack an extra punch, and not just in flavor. For most, eating moderate amounts fits just fine into a regular diet. The body breaks down tyramine mainly using an enzyme called monoamine oxidase, or MAO, found in the gut and liver.
Health and Tyramine—What’s the Link?
The story changes for people who rely on a type of antidepressant called MAO inhibitors (MAOIs). These medicines block the enzyme that processes tyramine. So if a person on MAOIs enjoys a big serving of aged cheese, tyramine can build up. This raises blood pressure so quickly that it can send someone straight to the ER with a hypertensive crisis. Signs like a pounding headache, flushing, rapid heartbeat, and sometimes chest pain can set in.
This is not just theory; real cases land in clinics every year. Some doctors still keep a “forbidden foods” list for patients starting MAOIs. A solid understanding of the risks makes it possible to manage depression with these older, sometimes more effective medications for tough cases, without causing avoidable trouble.
Beyond Depression: Migraines and Diet
Migraine sufferers sometimes notice that certain foods make headache days more frequent or severe. Tyramine stands out as a likely suspect. Those with sensitive systems may spot a pattern between cheese boards and pounding heads. While science on this link has twists and turns, it matches with many people’s experience: skip the aged cheese and get fewer headaches.
Advice for migraine-prone folks often includes a test of low-tyramine diets. Removing or limiting known offenders sometimes leads to relief that medicine alone cannot offer. For those affected, this sort of practical, food-based change makes living with a chronic condition more manageable.
Solutions and Education Matter
Labeling laws don’t always require a warning when foods are high in tyramine. Yet pharmacists and many doctors flag risk foods for anyone prescribed MAOIs. Self-education also goes a long way, and a trip to a registered dietitian can clear up big mysteries. In hospital settings, pharmacists have stepped up to keep preventable emergencies in check by tracking medications and counseling patients.
Food science still searches for better ways to predict and control tyramine levels in fermented products. Consumers could use more up-front information, but until then, awareness holds center stage. Those who know tyramine’s role—whether from lived experience or good counseling—find it far easier to dodge health scares and get the best use out of their meals and as-needed medications.
The Everyday Impact of Tyramine
Tyramine shows up in aged cheeses, smoked meats, some wines, and even soy products. Not everyone's heard of it, but people living with certain health conditions—especially those taking specific antidepressants—learn about it the hard way. For me, paying attention to tyramine wasn’t on my radar until a friend switched to an older antidepressant and, after eating a pizza with pepperoni and cheese, ended up in the emergency room with dangerously high blood pressure. That wakeup call taught me: not every ingredient in food plays nice with our bodies.
The Problem with Certain Medications
MAOIs, those older antidepressants, block the body’s normal handling of tyramine. When you eat tyramine-rich foods and are on these meds, blood pressure can spike fast. The science lines up with what I saw: hypertensive crisis, pounding headaches, sweating, chest pain, even risk of stroke. The reason is simple. Tyramine triggers the release of norepinephrine, a hormone that tightens blood vessels and lifts blood pressure. For people on MAOIs, stumbling onto a fancy cheese platter isn’t a minor issue—it can be life-threatening. Some healthcare providers skip these older drugs because of this diet hassle, but MAOIs still help people who don’t respond to other treatments, so the risk stays relevant.
Other Possible Reactions
Beyond medication risks, tyramine also stirs up migraines in susceptible folks. Foods heavy in tyramine have made their way onto lists that neurologists hand out to patients dealing with chronic headaches. While not everyone gets migraines from it, there’s good research showing tyramine can set off an episode for some. If you ever tried tracking food triggers for migraines, you know it’s not easy to pinpoint the exact culprit, but tyramine deserves a spot on the suspect list.
Why Tyramine Sensitivity Matters Today
Our culture has never been more in love with aged and fermented foods. Artisanal movements made things like cured meats, fancy cheeses, and pickled vegetables trendy. For most people, these foods are a pleasure; for a small crowd, they hide real danger. Food labels don’t shout out tyramine content, so there’s no shortcut to identifying risky items unless you already know what to look for. Plus, tyramine amounts differ from batch to batch, depending on how food is prepared and stored. This unpredictability creates a real problem for people trying to manage their intake.
What Can Be Done?
Doctors and dietitians play a central role, giving straight talk about what to avoid and what’s safe. Apps and online lists help, but nothing beats a direct conversation about risks and warning signs. Some patients carry wallet cards listing tyramine-rich foods, making it easier to check menus or shop for groceries. In my own circles, we’ve gone out of our way to flag risky foods at potlucks if we know someone needs to steer clear.
If you’re at risk—because of medication or migraines—connecting with your healthcare team, reading up on safe-eating guidelines, and letting friends and family know about your sensitivity truly matters. Tyramine usually flies under the radar, but for those affected, it’s not just about food preference—it’s about keeping safe and healthy.
Invisible Ingredient on the Plate
Tyramine doesn’t show up on most food labels, but its role in day-to-day health seems to get clearer year after year. Anyone stuck on certain medications—especially those with depression or Parkinson’s—hears about tyramine from a doctor sooner or later. It lives in favorites like aged cheese, cured meats, soy sauce, even some beers and wines. The trouble really starts with what happens inside the body, not on the dinner plate.
The MAOI Connection: Not Just a Warning Label
Monoamine oxidase inhibitors, often called MAOIs, treat some forms of depression and other neurological issues. These medications work well for the folks who need them, but the chemistry behind their effectiveness also flips a switch in how the body handles tyramine. Instead of breaking down quickly, tyramine piles up and comes on strong. High blood pressure can hit out of nowhere, landing people in the ER for what’s called a “hypertensive crisis.” A headache so intense it blinds you or a racing pulse that feels like panic – these aren’t rare stories in the medical journals. They keep happening due to a lack of awareness and gaps in the safety net of counseling and follow-up.
Food Choices That Matter
Grocery shopping and eating out take a new spin for anyone on these drugs. No more late-night pizza with extra pepperoni or an aged cheddar fix. Kombucha, a trendy “healthy” drink lately, sets off the same alarms. Fermented, aged, cured, or pickled often equals risky. I’ve seen friends switch diets overnight, scanning every bite for what could set off trouble. The stress is real and not often mentioned outside of clinical pamphlets.
Interactions Beyond MAOIs
Selegiline and rasagiline, used in Parkinson’s management, also open the door to dangerous spikes of tyramine. Some folks on other antidepressants report milder, less predictable forms of food sensitivity. Prescription drugs don’t come with a full menu plan, but maybe they should.
Lack of Standardized Food Labeling
No easy way exists for most shoppers to figure out which foods pack a tyramine punch. Online lists and hearsay help, but food labeling still falls short. In-person advice rarely goes beyond “avoid aged cheese.” Even nutritionists stumble over the specifics if they don’t regularly work with these cases. It leaves those at risk piecing together half-truths and hoping for the best.
Practical Ways Forward
Doctors and pharmacists already carry a heavy load, but real patient education could save lives. Candid talks about food swaps, lists taped to the fridge, or support from registered dietitians make a tangible difference. Digital apps that generate safe meal plans seem long overdue. I’d bet a solid collaboration between tech firms and clinical pharmacists could give at-risk patients direct, updated information before the next dangerous meal. Food producers could also step up, working with consumer safety groups to flag tyramine-rich products better, especially in specialty aisles and at delis.
Building Awareness
Tyramine’s effect stays niche outside the world of pharmacy shelves and academic papers. The risk doesn’t just belong to “old drugs” or far-off medical conditions. It circles around everyday eating, invisible, unless someone points it out. Spreading the word means less surprise and more control—for patients and families alike.
The Challenge of Tyramine for Certain People
Most folks don’t think twice about what’s in their cheese board or deli sandwich, but for some people, one ingredient hiding in aged and fermented foods causes real trouble: tyramine. This natural substance forms when protein breaks down, especially during aging or fermentation. You find it in old cheese, smoked fish, cured meats, soy products, draft beer, and even some overripe fruits.
Tyramine doesn’t bother most people. The problem kicks in for folks taking certain antidepressants—old drugs called monoamine oxidase inhibitors (MAOIs) like phenelzine, isocarboxazid, or tranylcypromine. If you’re on one of these, eating too much tyramine can send blood pressure rocketing, setting off pounding headaches, vision changes, and sometimes chest pain. The risk might seem rare, but I’ve seen firsthand how quickly a simple lunch can become an emergency. In one case, a friend with depression—who was new to his MAOI prescription—ate a pepperoni pizza and suffered a severe pressure headache that sent him to the ER. Once you live through something like that or witness it, you never take the subject lightly.
Who Has the Most to Lose?
This isn’t just about people taking prescription drugs. Anyone with high blood pressure, heart disease, chronic migraines, or those with known tyramine sensitivity also should tread carefully. A spike in blood pressure is dangerous business for someone whose heart or blood vessels are already on edge. In migraine patients, researchers have pointed to tyramine as a possible trigger, especially in recurring attacks. For people who struggle with migraines, relentless headaches disrupt work, family, and everything in between. Even without medication interactions, a plate of aged cheese can mean hours of agony or a trip to urgent care.
Doctor’s Advice—and Real-World Challenges
Doctors usually warn patients about this risk, but the real trap lies in everyday choices. Restaurants don’t label tyramine content. Store-bought soups, cured meats, and even leftovers can build up tyramine silently as they age. People may forget their doctor’s warning, thinking a small portion can’t do much harm. I’ve seen the same pattern repeat: someone feels good, gets overconfident, tries a risky food, and suffers. Once, during my pharmacy internship, a customer asked if “just a little blue cheese” was okay on her salad. She was shocked to learn that even small amounts could push her blood pressure too high.
Finding a Practical Path Forward
People need more than advice to eat fresh. Patients deserve clear instructions, plain-language lists of high-tyramine foods, and check-ins to review experiences. Pharmacies could make it standard to hand out wallet cards that name risky foods for anyone on MAOIs or with a migraine history. Smart grocery shopping—checking packaging dates, keeping food chilled, avoiding leftovers that sit for days—helps reduce accidental intake. Tech can help too. Nutrition apps could highlight tyramine-rich options if you enter your medication and health issues.
It helps when loved ones know what’s at stake. Friends and family can keep dangerous foods off the menu at gatherings. In workplaces or care homes, kitchen staff should get the memo. Preventing emergencies sometimes takes a village, especially if someone’s juggling multiple health concerns. Tyramine may seem like just another chemical, but for some people, it’s anything but harmless. Awareness, education, and practical habits make all the difference.
Tyramine sounds like a name you’d stumble upon in a science course rather than a conversation with your local pharmacist, but lately, it’s cropped up across fitness and nutrition circles. Some hope this compound, found in aged cheese, cured meats, and fermented foods, might offer perks as a supplement. Yet almost nobody talks straight about the right dose. If you ask online forums, you’ll hear everything from “just try what feels right” to “don’t touch it unless your doctor nods.” Health often struggles to squeeze into neat instructions, but the confusion around tyramine is on another level.
Why Tyramine Catches Attention
Tyramine sits in the group of so-called monoamine compounds. In the body, monoamine oxidase (MAO) enzymes normally take charge of tyramine from food. Trouble shows up when MAO is blocked by certain antidepressants—a surge in blood pressure can follow after eating too much tyramine. This “cheese effect” lands a starring role in medical textbooks, but what about folks turning to tyramine purposely, skipping the cheese platter and reaching for supplements?
What the Science Says About Dosage
Solid data on safe tyramine doses is thin. Research sticks mostly to tyramine in food, not pills or powders. Scientists know that as little as 6–10 mg of tyramine from food can trigger blood pressure spikes among people taking MAO inhibitors. The FDA flags tyramine as potentially harmful for some, but doesn’t hand out official supplement guidelines or recommended daily dosages. Medical journals stay clear of suggesting tyramine for any purpose, let alone giving a number to measure by spoon or capsule. That silence from authorities matters. If nobody's willing to call something safe above a certain point, the space between “a little” and “too much” gets risky.
Potential Harms and Missed Warnings
Most folks trying tyramine supplements aren’t on prescription MAOIs. That shouldn’t wave off all concerns. The body’s epinephrine and norepinephrine systems can still overreact. High blood pressure, headaches, and heart palpitations have kept ER doctors awake at night when people overconsume tyramine by mistake. Many supplements for energy or weight management quietly slip in tyramine without explaining the risks. This lack of labeling frustrates anyone hoping to make informed choices.
The Call for Common Sense and Clearer Rules
Close friends have asked if tyramine might boost workouts or sharpen focus. I always say the same thing: right now, nobody can state a safe, recommended dose—because the data just isn’t there. Self-experimentation is tempting, but blood pressure isn’t something to play roulette with.
Medical communities and supplement brands need to be honest about unknowns. Screening and labeling should spell out if a product contains tyramine and warn those with heart problems, headaches, or those taking sensitive medications. Instead of searching for some magic bullet in new supplements, energy seekers do better to focus on sleep, nutrition, and movement—old approaches that have always worked better than chasing a shortcut through a pill.
Until smarter research and honest oversight step in, tyramine supplements stay in murky territory. No one should gamble their health on an unregulated product that nobody can assign a safe limit to—not today, and not tomorrow.